|
In Greek, athere means gruel, and skleros means hard. Atherosclerosis is often called arteriosclerosis. Arteriosclerosis (from the Greek arteria, meaning artery) is a general term for hardening of the arteries. Arteriosclerosis can occur in several forms, including atherosclerosis. Description. Atherosclerosis, a progressive process responsible for most heart disease, is a type of arteriosclerosis or hardening of the arteries. 
Key facts & figures Coronary Heart Disease remains the number 1 killer in the UK. Deaths In the UK every year. 160,000 people die from heart and circulatory disease. An artery is made up of several layers: an inner lining called the endothelium, an elastic membrane that allows the artery to expand and contract, a layer of smooth muscle, and a layer of connective tissue. Arteriosclerosis is a broad term that includes a hardening of the inner and middle layers of the artery. It can be caused by normal aging, by high blood pressure, and by diseases such as diabetes. Atherosclerosis is a type of arteriosclerosis that affects only the inner lining of an artery. It is characterized by plaque deposits that block the flow of blood. Plaque is made of fatty substances, cholesterol, waste products from the cells, calcium, and fibrin, a stringy material that helps clot blood. The plaque formation process stimulates the cells of the artery wall to produce substances that accumulate in the inner layer. Fat builds up within these cells and around them, and they form connective tissue and calcium. The inner layer of the artery wall thickens, the artery's diameter is reduced, and blood flow and oxygen delivery are decreased. Plaques can rupture or crack open, causing the sudden formation of a blood clot (thrombosis). Atherosclerosis can cause a heart attack if it completely blocks the blood flow in the heart (coronary) arteries. It can cause a stroke if it completely blocks the brain (carotid) arteries. Atherosclerosis can also occur in the arteries of the neck, kidneys, thighs, and arms, causing kidney failure or gangrene and amputation. Original Article. Prevention of Coronary Heart Disease with Pravastatin in Men with Hypercholesterolemia. James Shepherd, M.D., Stuart M. Cobbe, M.D., Ian Ford, Ph.D. Cholesterol, from the Ancient Greek chole- and stereos (solid) followed by the chemical suffix-ol for an alcohol, is an organic molecule. It is a sterol (or modified. Atherosclerosis (also known as arteriosclerotic vascular disease or ASVD) is a specific form of arteriosclerosis in which an artery wall thickens as a result of. Learn about atherosclerosis and heart disease prevention, natural treatments, home remedies. I25.1 is not a billable or specific ICD-10-CM diagnosis code as there is 1 code below I25.1 that describe this diagnosis in greater detail. This is the American ICD. Causes and symptoms. Atherosclerosis can begin in the late teens, but it usually takes decades to cause symptoms. Some people experience rapidly progressing atherosclerosis during their thirties, others during their fifties or sixties. 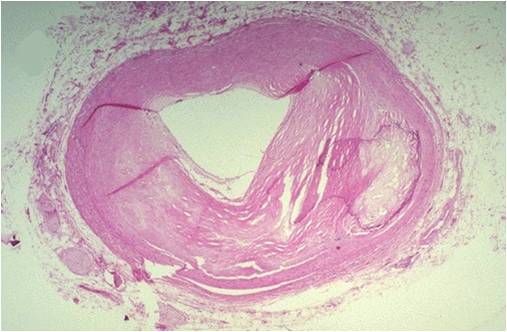
Learn about Zocor (Simvastatin) may treat high cholesterol and triglyceride levels, uses, dosage, side effects, risk, drug interactions, warnings, patient labeling. Rapid growth and technologic. Then, I’ll bet that you landed here because you are looking for some real CholesLo reviews – so you can make an informed decision whether this lowering. Free cholesterol papers, essays, and research papers. These results are sorted by most relevant first (ranked search). You may also sort these by color rating or.  
Atherosclerosis is complex. Its exact cause is still unknown. It is thought that atherosclerosis is caused by a response to damage to the endothelium from high cholesterol, high blood pressure, and cigarette smoking. A person who has all three of these risk factors is eight times more likely to develop atherosclerosis than is a person who has none. Physical inactivity, diabetes, and obesity are also risk factors for atherosclerosis. High levels of the amino acid homocysteine and abnormal levels of protein- coated fats called lipoproteins also raise the risk of coronary artery disease. These substances are the targets of much current research. 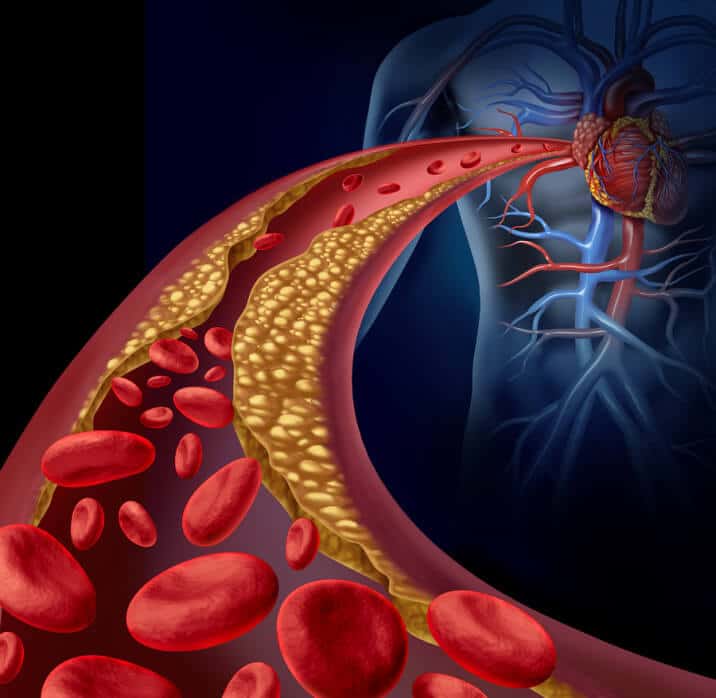 
The role of triglycerides, another fat that circulates in the blood, in forming atherosclerotic plaques is unclear. High levels of triglycerides are often associated with diabetes, obesity, and low levels of high- density lipoproteins (HDL cholesterol). The more HDL (. These risk factors are all modifiable. Non- modifiable risk factors are heredity, sex, and age. Risk factors that can be changed: Cigarette/tobacco smoke- Smoking increases both the chance of developing atherosclerosis and the chance of dying from coronary heart disease. Second hand smoke may also increase risk. High blood cholesterol- Cholesterol, a soft, waxy substance, comes from foods such as meat, eggs, and other animal products and is produced in the liver. Age, sex, heredity, and diet affect cholesterol. 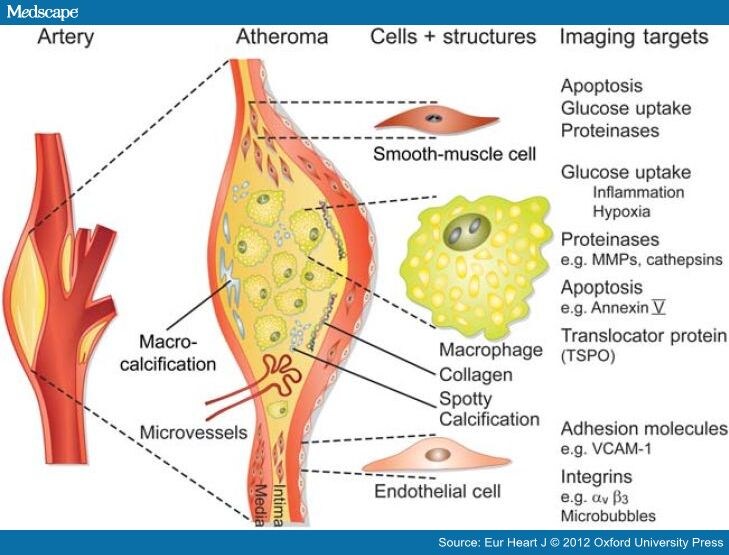
Total blood cholesterol is considered high at levels above 2. L and borderline at 2. L. High- risk levels of low- density lipoprotein (LDL cholesterol) begin at 1. L. High triglycerides- Most fat in food and in the body takes the form of triglycerides. Blood triglyceride levels above 4. 
L have been linked to coronary artery disease in some people. Triglycerides, however, are not nearly as harmful as LDL cholesterol. High blood pressure- Blood pressure of 1. Physical inactivity- Lack of exercise increases the risk of atherosclerosis. Diabetes mellitus- The risk of developing atherosclerosis is seriously increased for diabetics and can be lowered by keeping diabetes under control. Most diabetics die from heart attacks caused by atherosclerosis. Obesity- Excess weight increases the strain on the heart and increases the risk of developing atherosclerosis even if no other risk factors are present. 
Risk factors that cannot be changed: Heredity- People whose parents have coronary artery disease, atherosclerosis, or stroke at an early The progression of atherosclerosis.(Illustration by Hans & Cassady.)age are at increased risk. The high rate of severe hypertension among African- Americans puts them at increased risk. Sex- Before age 6. After age 6. 0, the risk is equal among men and women. Age- Risk is higher in men who are 4. Symptoms differ depending upon the location of the atherosclerosis. In the coronary (heart) arteries: Chest pain, heart attack, or sudden death. In the carotid (brain) arteries: Sudden dizziness, weakness, loss of speech, or blindness. In the femoral (leg) arteries: Disease of the blood vessels in the outer parts of the body (peripheral vascular disease) causes cramping and fatigue in the calves when walking. In the renal (kidney) arteries: High blood pressure that is difficult to treat. Diagnosis. Physicians may be able to make a diagnosis of atherosclerosis during a physical exam by means of a stethoscope and gentle probing of the arteries with the hand (palpation). More definite tests are electrocardiography, echocardiography or ultrasonography of the arteries (for example, the carotids), radionuclide scans, and angiography. An electrocardiogram shows the heart's activity. Electrodes covered with conducting jelly are placed on the patient's body. They send impulses of the heart to a recorder. The test takes about 1. Exercise electrocardiography (stress test) is conducted while the patient exercises on a treadmill or a stationary bike. It is performed in a physician's office or an exercise laboratory and takes 1. Echocardiography, cardiac ultrasound, uses sound waves to create an image of the heart's chambers and valves. A technician applies gel to a hand- held transducer, presses it against the patient's chest, and images are displayed on a monitor. This technique cannot evaluate the coronary arteries directly. They are too small and are in motion with the heart. Severe coronary artery disease, however, may cause abnormal heart motion that is detected by echocardiography. Performed in a cardiology outpatient diagnostic laboratory, the test takes 3. Ultrasonography is also used to assess arteries of the neck and thighs. Radionuclide angiography and thallium (or sestamibi) scanning enable physicians to see the blood flow through the coronary arteries and the heart chambers. Radioactive material is injected into the bloodstream. A device that uses gamma rays to produce an image of the radioactive material (gamma camera) records pictures of the heart. Radionuclide angiography is usually performed in a hospital's nuclear medicine department and takes 3. Thallium scanning is usually done after an exercise stress test or after injection of a vasodilator, a drug to enlarge the blood vessels, like dipyridamole (Persantine). Thallium is injected, and the scan is done then and again four hours (and possibly 2. Thallium scanning is usually performed in a hospital's nuclear medicine department. Each scan takes 3. Coronary angiography is the most accurate diagnostic method and the only one that requires entering the body (invasive procedure). A cardiologist inserts a catheter equipped with a viewing device into a blood vessel in the leg or arm and guides it into the heart. The patient has been given a contrast dye that makes the heart visible to x rays. Motion pictures are taken of the contrast dye flowing though the arteries. Plaques and blockages, if present, are well defined. The patient is awake but has been given a sedative. Coronary angiography is performed in a cardiac catheterization laboratory and takes from 3. Treatment. Treatment includes lifestyle changes, lipid- lowering drugs, percutaneous transluminal coronary angioplasty, and coronary artery bypass surgery. Atherosclerosis requires lifelong care. Patients who have less severe atherosclerosis may achieve adequate control through lifestyle changes and drug therapy. Many of the lifestyle changes that prevent disease progression- a low- fat, low- cholesterol diet, losing weight (if necessary), exercise, controlling blood pressure, and not smoking- also help prevent the disease. Key terms. Arteriosclerosis — Hardening of the arteries. It includes atherosclerosis, but the two terms are often used synonymously. Cholesterol — A fat- like substance that is made by the human body and eaten in animal products. Cholesterol is used to form cell membranes and process hormones and vitamin D. High cholesterol levels contribute to the development of atherosclerosis. HDL Cholesterol — About one- third or one- fourth of all cholesterol is high- density lipoprotein cholesterol. High levels of HDL, nicknamed . High levels of LDL, nicknamed . Elevated triglyceride levels contribute to the development of atherosclerosis. Most of the drugs prescribed for atherosclerosis seek to lower cholesterol. Many popular lipid- lowering drugs can reduce LDL- cholesterol by an average of 2. Lipid- lowering drugs include bile acid resins, . Aspirin helps prevent thrombosis and a variety of other medications can be used to treat the effects of atherosclerosis. Percutaneous transluminal coronary angioplasty and bypass surgery are invasive procedures that improve blood flow in the coronary arteries. Percutaneous transluminal coronary angioplasty (coronary angioplasty) is a non- surgical procedure in which a catheter tipped with a balloon is threaded from a blood vessel in the thigh into the blocked artery. Uses, Side Effects, Drug Interactions, Dosage & Warnings. WARNINGSIncluded as part of the PRECAUTIONS section. PRECAUTIONSMyopathy/Rhabdomyolysis. Simvastatin occasionally causes myopathy manifested as. CK) above ten times. ULN). Myopathy sometimes takes the form of. The risk of myopathy is increased by high. Predisposing factors for myopathy include. In a clinical trial database in which 4. ZOCOR, 2. 4,7. 47 (approximately 6. The incidence. of myopathy with 8. In these trials, patients were carefully monitored and some. In a clinical trial in which 1. ZOCOR (mean follow- up 6. The incidence of rhabdomyolysis (defined as myopathy. CK > 4. 0 times ULN) in patients on 8. The incidence of myopathy. In this trial, patients. The risk of myopathy, including rhabdomyolysis, is. LDL- C- lowering efficacy and compared with lower doses. Therefore, the 8. ZOCOR should be used only in. If, however, a patient who is. ZOCOR needs to be initiated on an. Patients should be advised of the increased risk. If symptoms occur, treatment should be. IMNM is characterized by: proximal muscle weakness and elevated serum. All patients starting therapy with ZOCOR, or whose. ZOCOR is being increased, should be advised of the risk of myopathy. ZOCOR. ZOCOR therapy. In. most cases, muscle symptoms and CK increases resolved when treatment was. Periodic CK determinations may be considered in patients. ZOCOR or whose dose is being increased, but there is no assurance. Many of the patients who have developed rhabdomyolysis on. Such patients merit closer monitoring. ZOCOR therapy should be. CPK levels occur or myopathy is diagnosed or. ZOCOR therapy should also be temporarily withheld in any patient. Drug Interactions. The risk of myopathy and rhabdomyolysis is increased by. Simvastatin is metabolized by the. P4. 50 isoform 3. A4. Certain drugs which inhibit this metabolic pathway. These include itraconazole, ketoconazole, posaconazole, voriconazole. HIVprotease inhibitors, boceprevir, telaprevir, the. Combination of these drugs with simvastatin is. If short- term treatment with strong CYP3. A4 inhibitors is. In an ongoing, double- blind, randomized. Chinese compared with. Chinese patients taking simvastatin 4. Caution should be used when. Chinese patients with simvastatin in doses exceeding 2. Because. the risk for myopathy is dose- related, Chinese patients should not receive. It is unknown if the risk for myopathy with coadministration of. Chinese patients applies to other Asian patients . When drug treatment was interrupted or. The increases were not associated with jaundice or other clinical signs. There was no evidence of hypersensitivity. In the Scandinavian Simvastatin Survival Study (4. S) . Of the 1,9. 86 simvastatin treated patients in 4. S with normal liver. LFTs) at baseline, 8 (0. LFT. elevations to > 3. X ULN and/or were discontinued due to transaminase. Among these 8. patients, 5 initially developed these abnormalities within the first year. All. of the patients in this study received a starting dose of 2. In 2 controlled clinical studies in 1,1. There have been rare postmarketing reports of fatal and. If. serious liver injury with clinical symptoms and/or hyperbilirubinemia or. ZOCOR, promptly interrupt therapy. If an. alternate etiology is not found do not restart ZOCOR. Note that ALT may emanate. ALT rising with CK may indicate myopathy . Active liver diseases or unexplained transaminase elevations are contraindications. Moderate (less than 3. X ULN) elevations of serum. These. changes appeared soon after initiation of therapy with simvastatin, were often. Endocrine Function. Increases in Hb. A1c and fasting serum glucose levels have. HMG- Co. A reductase inhibitors, including ZOCOR. Nonclinical Toxicology. Carcinogenesis, Mutagenesis, Impairment Of Fertility. In a 7. 2- week carcinogenicity study, mice were. AUC) after an 8. 0- mg oral dose. Liver carcinomas were. The incidence of adenomas of the liver was. Drug treatment also. Adenomas of the Harderian gland (a gland of the eye of. No. evidence of a tumorigenic effect was observed at 2. In a separate 9. 2- week carcinogenicity study in mice at. AUC). In a two- year study in rats at 2. AUC). A second two- year rat carcinogenicity study with doses of. Thyroid follicular cell. The increased. incidence of thyroid neoplasms appears to be consistent with findings from. These treatment levels represented plasma drug levels (AUC) of. No evidence of mutagenicity was observed in a microbial. Ames) test with or without rat or mouse liver metabolic. In addition, no evidence of damage to genetic material was noted in. V- 7. 9 mammalian cell. CHO cells. or an in vivo chromosomal aberration assay in mouse bone marrow. There was decreased fertility in male rats treated with. AUC, in patients receiving 8. No. microscopic changes were observed in the testes of rats from either study. At. 1. 80 mg/kg/day, (which produces exposure levels 2. In. dogs, there was drug- related testicular atrophy, decreased spermatogenesis. AUC, at 8. 0 mg/day). The. clinical significance of these findings is unclear. Use In Specific Populations. Pregnancy. Pregnancy Category X . Lipid lowering drugs offer no benefit during pregnancy, because. There are no adequate and. ZOCOR during pregnancy; however, there are. Serum cholesterol and triglycerides increase during. Because statins decrease cholesterol synthesis and possibly. ZOCOR may cause fetal harm when administered to a pregnant woman. If ZOCOR is. used during pregnancy or if the patient becomes pregnant while taking this. There are rare reports of congenital anomalies following. In a review. 2 of approximately 1. However, the study was only able to exclude a 3- to 4- fold. In 8. 9% of these. Simvastatin was not teratogenic in rats or rabbits at. However, in studies with another structurally- related. Women of childbearing potential, who require treatment. ZOCOR for a lipid disorder, should be advised to use effective. For women trying to conceive, discontinuation of ZOCOR should be. If pregnancy occurs, ZOCOR should be immediately discontinued. Nursing Mothers. It is not known whether simvastatin is excreted in human. Because a small amount of another drug in this class is excreted in human. A decision. should be made whether to discontinue nursing or discontinue drug, taking into. Patients treated with simvastatin had an adverse. Doses. greater than 4. In this limited. controlled study, there was no significant effect on growth or sexual maturation. Simvastatin has not been studied in patients younger than 1. Geriatric Use. Of the 2,4. ZOCOR in Phase III. Heart Protection Study who. ZOCOR, 3. 63 (1. 5%) and 5,3. No overall differences in safety or. Since advanced age ( . In 4. S, 1,0. 21 (2. Lipid- lowering efficacy. ZOCOR significantly reduced total mortality and CHD mortality in elderly. CHD. In HPS, 5. 2% of patients were elderly (4,8. The relative risk. CHD death, non- fatal MI, coronary and non- coronary. In HPS, among 3. 2,1. Of the 7 cases of myopathy/rhabdomyolysis among. There were no overall differences in safety between. S or HPS. Because advanced age ( . In a clinical trial of patients treated with simvastatin.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
